Understanding covid-19’s role in promoting quackery. The escalated demand for expansive “immunity boosters” and other forms of natural medicines are indicating that the coronavirus pandemic has created a huge market for alternative medicine.
By Abhijit Chanda

WITH the COVID-19 pandemic came another, which spread even faster–misinformation. Most of it was regarding complementary and alternative medicine (CAM) and fake cures in email forwards, WhatsApp messages, YouTube videos, newspaper articles and even government promotion. The question that remains is, why? Isn’t this a time when people should be more motivated to heed medical experts and authorities? Today, we look for answers.
LOSS OF FAITH IN MEDICINE
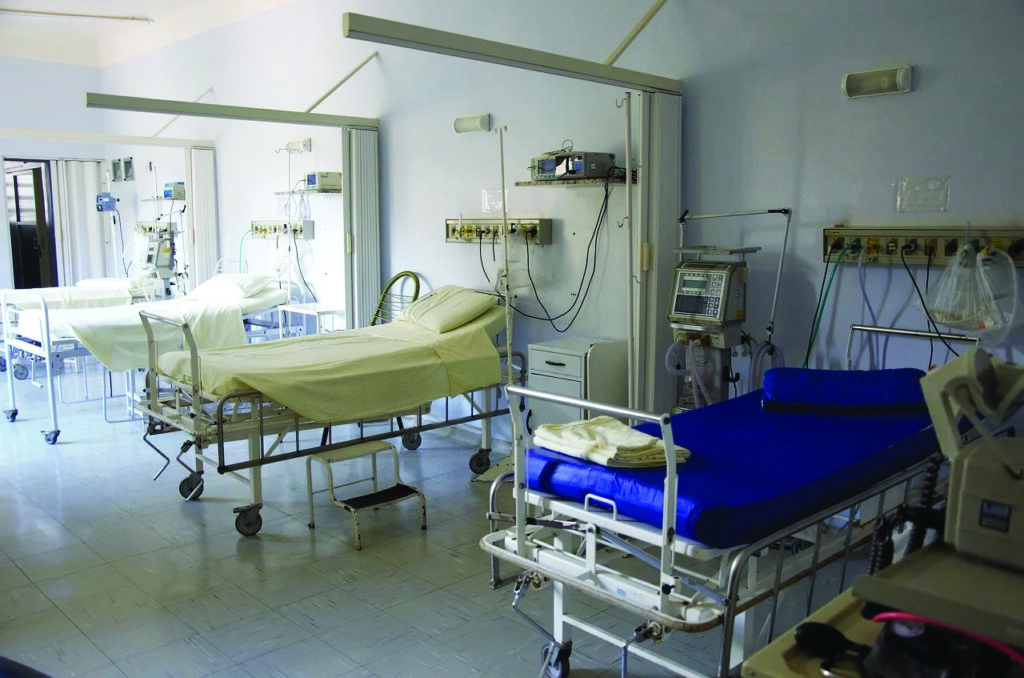
More expensive private hospitals have grown in popularity. Still, they are notorious for charging exorbitant rates for diagnostic tests and even medical treatments. Hospital rooms can often be more expensive than hotel rooms. For instance, a private room in New Delhi can cost Rs. 5,000 up to Rs. 70,000. The common person can’t afford those kinds of rates. On the other hand, public hospitals with subsidized rates are often understaffed and overburdened by patients. The hygiene levels are notoriously horrible in most government hospitals too. A common sight in such facilities is rust-eaten beds, paan stains on walls, dirty sheets and rats, a lack of toilets, let alone clean ones, and other horrors.
Adding to that, the number of doctors needed for our population still hasn’t touched the WHO recommendations of 1 doctor to 1,000 people. Some hopeful predictions say we might reach that target in 2024, but that depends on how seriously our medical colleges and infrastructure try to retain medical professionals in our country. After all, many doctors are more willing to migrate to a developed country than practice in India.
As of 2017, more than 15,000 doctors completed their studies in medicine in India and are now in the NHS, UK. Also, as of early 2019, Indians represented a majority among non-British nationalities for NHS staff.
According to an article published in The Public Health Advocate, University of Berkeley, by Kavya Venkat, “India faces a health workforce crisis. According to the WHO, the doctor-to-patient ratio is 1:10,000. A recent study in Public Health found that, on average, the government hired doctors within the country to attend to more than 10,000 people, which is almost 10 times more than the recommended number for physicians. Th is leads to burnout for current healthcare professionals. With the increase in population size, India requires a stronger healthcare foundation. With their already inadequate infrastructure and human resources, they struggle to serve many people in need. Even with an increase in medical colleges, India cannot sustain itself due to the massive size of the population, and migration of doctors to developed countries, such as the US, does not help their current state either.” She continues: “While around 600,000 physicians are registered to practice within India, the actual number is much less due to emigration. In addition, the number of physicians in rural versus urban areas is very skewed towards urban areas (there are almost 6 times more doctors in urban areas).” Indeed, in rural India, modern medicine is even harder to access.
According to a paper in Public Health in Practice by Anant Kumar et al. in November 2020, “The Indian rural health care system is a three-tier system comprising Sub-Centres, Primary Health Centres (PHC), and Community Health Centres (CHC). There is currently a shortfall in health facilities: 18% at the Sub-Centre level, 22% at the PHC level and 30% at the CHC level (as of March 2018)” Furthermore, the data presented in the Key Indicators of Social Consumption in India – Health, 2014, in the 2019 National Health Profile is even more troubling. The study found that the average number of government beds available per 10,000 people in rural India is just 3.2. Many states are much lower than this national average. For instance, Maharashtra has 2, and Bihar has only .6 beds per 10,000 people.
It’s not surprising that Indians have a lot of reasons to be disenchanted by modern medicine when the medical infrastructure in our country is so deeply flawed and woefully inadequate.
THE STUDY FOUND THAT THE AVERAGE NUMBER OF GOVERNMENT BEDS AVAILABLE PER 10,000 PEOPLE IN RURAL INDIA IS JUST 3.2. MANY STATES ARE MUCH LOWER THAN THIS NATIONAL AVERAGE
ALTERNATIVE IN INDIAN CULTURE
So people turn to alternative medicine because it’s seen as a part of our culture for millennia. Ayurveda has been an integral part of Indian culture since the Vedic period, around the second century BC. Siddha is also a traditional system of medicine (TSM) prominent in southern India, and Unani originating in Greece, and brought into India first by Alexander the Great and promoted under the Mughal empire. These TSMs are similar in that they are based on natural herbs, oils and minerals to create medicines.
Homoeopathy was invented by a German called Samuel Hahnemann. It was brought into India by various people who had seen it in Europe. It first took hold in West Bengal and has become a well-respected form of alternative medicine after Ayurveda.
It is important to note that all these TSMs were created before modern medical science came to be today. None of them holds up to the scientific rigour medicines have to go through today. Homoeopathy is based on Hahnemann’s principle that cures like – that a substance causing specific symptoms can cure the disease that causes them if it’s diluted enough. Many homoeopathic recommendations are made by diluting a substance so thoroughly that there is barely any chance that even a single molecule of the original compound remains.
The claim that this distilled water can cure any disease goes against the laws of physics, chemistry and biology. And yet, homoeopathy has been researched in great detail, with over 1,800 studies to its name. Repeatedly, it’s been found that homoeopathy is no more effective than a placebo. They are literally sugar pills. Somehow, it remains prevalent in India as it is touted as a treatment with no side effects or effects to speak of. Ayurveda, Siddha and Unani also originated long before double-blinded, placebo-controlled clinical trials existed.
They were developed through trial and error, with no care taken to note side effects, the placebo effect, cognitive biases or any other variables that may lead to mistaken findings. Notably, these variables are always considered when studying modern medicine. First, there are lab tests to see if candidate compounds have the desired effect in a test tube or a Petri dish. The animal trials are conducted to see the effects and side effects in mice or other rodents. Only when the molecule successfully comes through these tests and proves itself safe and effective is it tested on progressively larger groups of humans. These tests are:
Randomised: A random collection of people across genders and of specific agegroups or certain levels or health, or with a particular illness are divided into groups, so the results represent a certain population.
Placebo-controlled: One group is given the medicine, and the control group is given a placebo to see if the treatment has a significant effect.
Double-blinded: Neither the candidates nor the researchers know which group got the placebo and which got the active molecule so that there is no chance for bias from either side. That’s what gives this form of research its name of being a randomized controlled trial (RCT).
As an extra precaution, a research paper needs to be peer-reviewed, meaning it needs to be checked by an unbiased party to ensure the data was correctly collected and the results are accurate before it’s published in a reputed journal. Without these steps, it’s impossible to control all the variables that could contribute to a patient feeling better. Alternative medicine researchers haven’t yet incorporated these practices into their research, at least not faithfully.
Take, for example, the Corona Kit by Patanjali. They claimed the kit was prepared scientifically and 100% effective! There is no treatment in modern medicine that is 100% effective. That, in itself, is a red flag.

Edzard Ernst, MD, PhD and author of Trick or Treatment, had these questions of the study:
1) Why do the authors call it a pilot study? A pilot study is merely for testing the feasibility of a trial design and is not meant to yield definitive efficacy results
2) The authors state that the patients were asymptomatic yet in the discussion they claim they were asymptomatic or mildly symptomatic.
3) Some of the effect sizes reported here are extraordinary and seem almost too good to be true.
4) The claim of no adverse effect is implausible; even placebos would cause perceived adverse effects in a percentage of patients.
5) If the study is solid and withstands the scrutiny of the raw data, it is of huge relevance for public health.
So, why did the authors publish it in PHYTOMEDICINE, a relatively minor and little-known journal?”
Patanjali was ridiculed quite a bit for pushing this “cure” for COVID, not only because their “pilot” study was riddled with holes, but because it was such an obvious money grab. They found an opportunity and took it, with their products hitting the shelves of Patanjali stores nationwide without the necessary paperwork needed. Dr Harsh Vardhan, former Union Minister for Health & Family Welfare, even attended the launch event for Coronil Kit. Patanjali finally lowered its claims to make the Coronil Kit just a prophylactic, for which there still isn’t any evidence.
ENDORSEMENTS OF CAM
As soon as COVID-19 reached India, the government or, more specifically, the Ministry of AYUSH (Ayurveda, Yoga, Unani, Siddha, Homoeopathy and Naturopathy) started releasing notices recommending a variety of Ayurvedic, Unani, Homoeopathy and Siddha preparations to minimise chances of being infected with the virus. For example, Arsenicum Album was promoted to prevent infection from COVID-19 along with Ashwagandha, Chyawanprash, turmeric, giloy and even oil pulling.
After all, SARS-CoV-2 is a novel coronavirus, meaning it has never been encountered before and therefore has no known cure. How could ancient medical systems have anticipated such a disease and had preparations ready? Since there is no evidence to support any of the claims made, they haven’t.
Through the whole pandemic, the Ministry of AYUSH published tons of promotional materials on social media to promote the uses of these so-called medicines, giving a sheen of credibility to their claims since it’s a government organisation.
The Ministry is growing every year, with lots of support from the centre. The latest Union Budget has allocated Rs. 3,050 crores to the ministry for the coming year. On the other hand, the proposed expenditure on public health has dropped by 45% this year! The government wants to spend Rs 41,011 crore in 2022-23, while its expenses in the current financial year was Rs 74,820 – a move hard to believe or understand while we are still in the middle of a raging pandemic.
AND FINALLY, FEAR!
The Indian public has a deep cultural connection to alternative medicine, more often than not, believing it to be as scientific as modern medicine, or even more so. These medicines have been given along with mainstream medicine ever since they came into being, thereby earning their name as Complementary and Alternative Medicines.
However, the fear of this unknown disease with unknown treatments has possibly served as a catalyst that has led people to grasp whatever treatments they feel they can believe in. With no mainstream medicines to complement, these medicines have taken the pole position in people’s minds when treating or preventing COVID.
Along with the treatments mentioned above, people have been frantically doing steam inhalation, eating garlic and drinking milk with turmeric, along with any remedies they see on Whatsapp and emails like Vitamins D and C, zinc supplements, Ivermectin and so on, none of which have been proven to do anything at all to prevent or treat the coronavirus. The market is also filled with a slew of other products that promise to “boost immunity”, even though there is no such thing. The only natural way to boost your immunity without causing an autoimmune disease is to get vaccinated, which, fortunately, most people are doing.
And yet, there is a rise in vaccine hesitancy as well. But that’s a story for another time. A raging pandemic and scared people brought out quacks and charlatans, governments and social media influencers, brands, businesses and celebrities to tout their special magic potion to cure us. Wouldn’t we all be so much better off if these potions did work and ward off this horrible pandemic? I, for one, wish all their claims were true. But unfortunately, when something sounds too good to be true, it usually is.
